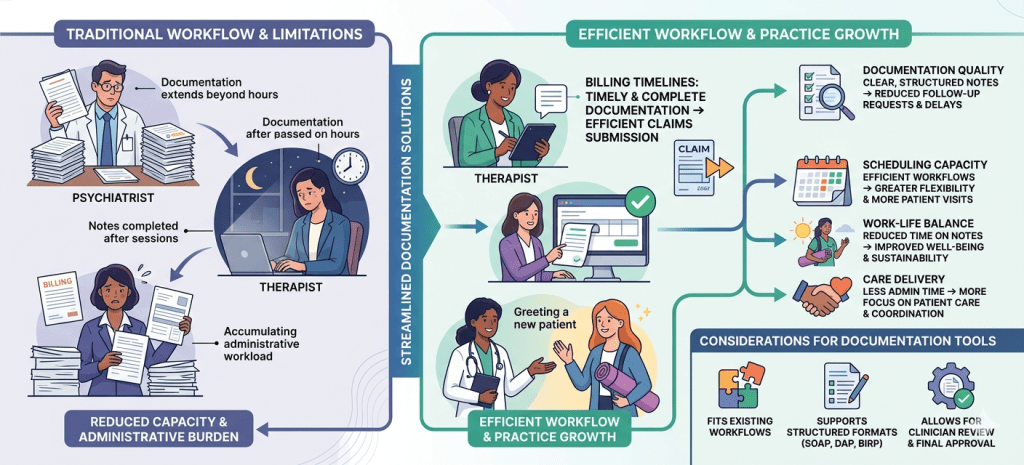
In many mental health practices, documentation is often viewed primarily as a compliance requirement. However, documentation workflows can also influence operational efficiency, billing timelines, and overall practice capacity.
As administrative demands increase, many clinicians are exploring tools and processes that may help streamline documentation while maintaining clinical quality and regulatory standards.
Time spent on documentation is a necessary part of care delivery, but it can also affect how clinicians structure their day.
For many psychiatrists, psychiatric nurse practitioners, and therapists:
These patterns can contribute to:
Timely and complete documentation can help support more efficient claims submission.
Clear, structured notes may reduce the likelihood of follow-up requests or delays during the billing process.
When documentation workflows are more efficient, clinicians may have greater flexibility in managing their schedules.
Even modest changes in documentation time can influence day-to-day operations. For example:
Results will vary by practice, and outcomes depend on multiple factors including patient population, visit type, and operational structure.
Not all documentation tools are designed specifically for mental health workflows.
Behavioral health documentation often requires:
Tools that are not designed for these use cases may require additional editing or manual input.
When evaluating documentation support tools, mental health providers may consider whether the system:
Documentation should always be reviewed and finalized by a licensed clinician to ensure accuracy, completeness, and compliance with applicable standards.
As mental health care evolves, particularly in telehealth and distributed care models, there is increasing focus on operational efficiency alongside clinical quality.
Documentation workflows are one area where improvements may support:
Efficient documentation not only saves time but also supports smoother operations across scheduling, billing, and care delivery.
For mental health providers, the goal is not to reduce the importance of documentation, but to ensure it is completed in a way that is accurate, compliant, and aligned with clinical workflows.
Tools designed to support documentation may play a role in that process, when implemented thoughtfully and used alongside appropriate clinical oversight.