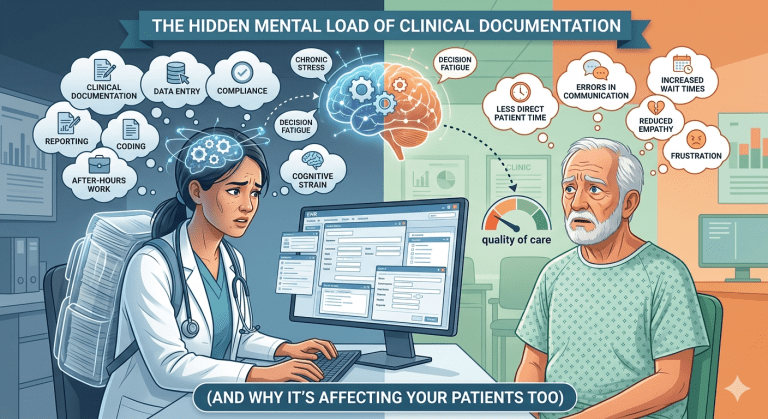
It’s not just charting. It’s cognitive residue. Most conversations around documentation focus on time:
But what gets missed is something deeper: What documentation does to your brain while you’re still in the room.
In mental health, presence is everything. But documentation forces a constant internal split:
That’s not just multitasking, that’s cognitive fragmentation and over time, it adds up.
Studies on AI scribes show reduced cognitive load and documentation burden when clinicians are freed from this mental overhead.
Because the real issue isn’t just time, it’s attention.
When documentation becomes the dominant task, it starts to change how clinicians work:
No one teaches this, but it happens anyway.
Patients don’t see your notes. But they feel when your attention shifts.
They notice:
Even small disruptions matter in mental health care, because trust is built in the margins.
Documentation doesn’t stay at work. It follows you home.
This is where burnout compounds. Not just from hours worked, but from mental carryover.
Most tools try to make documentation:
All important. But they miss the real question: Does this reduce the mental weight of the work?
Because clinicians aren’t just overloaded with tasks. They’re overloaded with context switching, pressure, and cognitive strain.
The shift isn’t about better templates. It’s about removing documentation from the cognitive foreground entirely. That’s where ambient AI documentation comes in:
Instead of thinking:
“What do I need to write down?”
You can think:
“What does this patient actually need right now?”
Ambient documentation systems are designed specifically to reduce manual data entry and improve clinician focus during encounters.
Yes, reducing documentation time matters. But the real impact is:
And those things compound. Because when clinicians feel better, care gets better.
Documentation isn’t just an administrative task, it’s a cognitive load problem, a mental health problem and ultimately, a patient care problem.
Most clinicians don’t say this out loud. But they feel it every day. And it doesn’t have to stay that way.
PMHScribe was built to remove documentation from your mental bandwidth, not just your schedule.
One conversation.
One click.
Your note is done.